Our Hospitals Transformation Programme
Opening in 2028, our exciting multi-million pound investment in our hospitals will benefit all our patients
What we’re doing
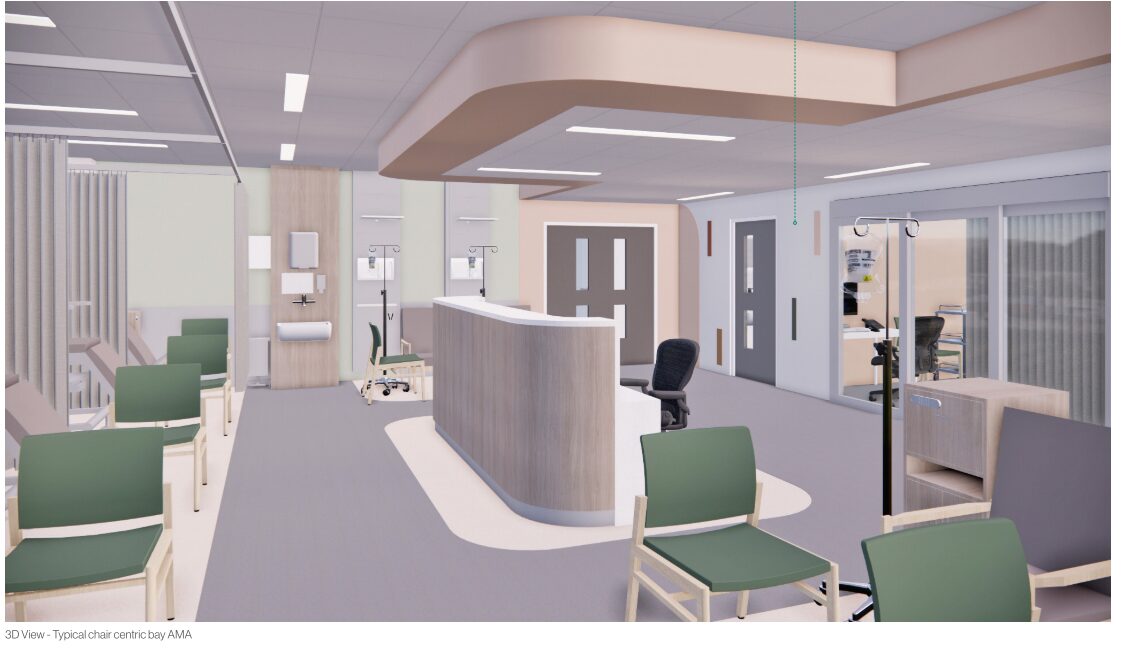
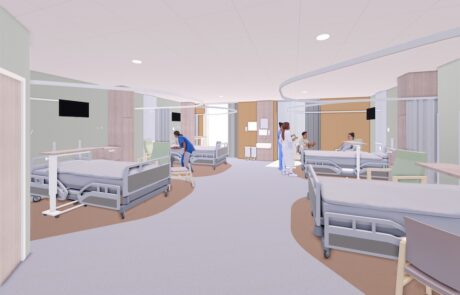
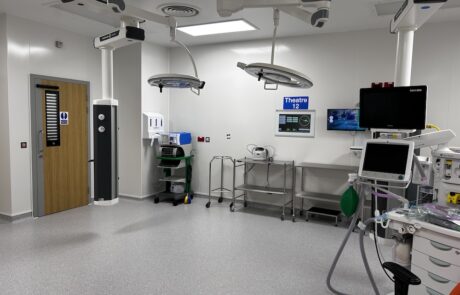
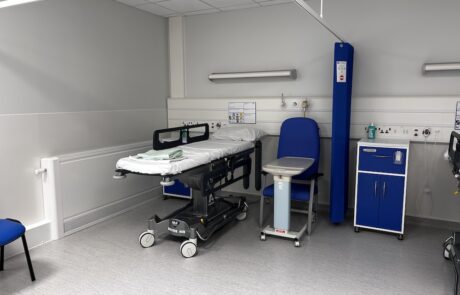
Our multi-million pound investment will improve care for everyone through modern, purpose-built facilities and ensure more people get the care they need, at the right time and in the right place. These plans have been led by our doctors and nurses to develop two thriving hospitals, supported by more services in the community.
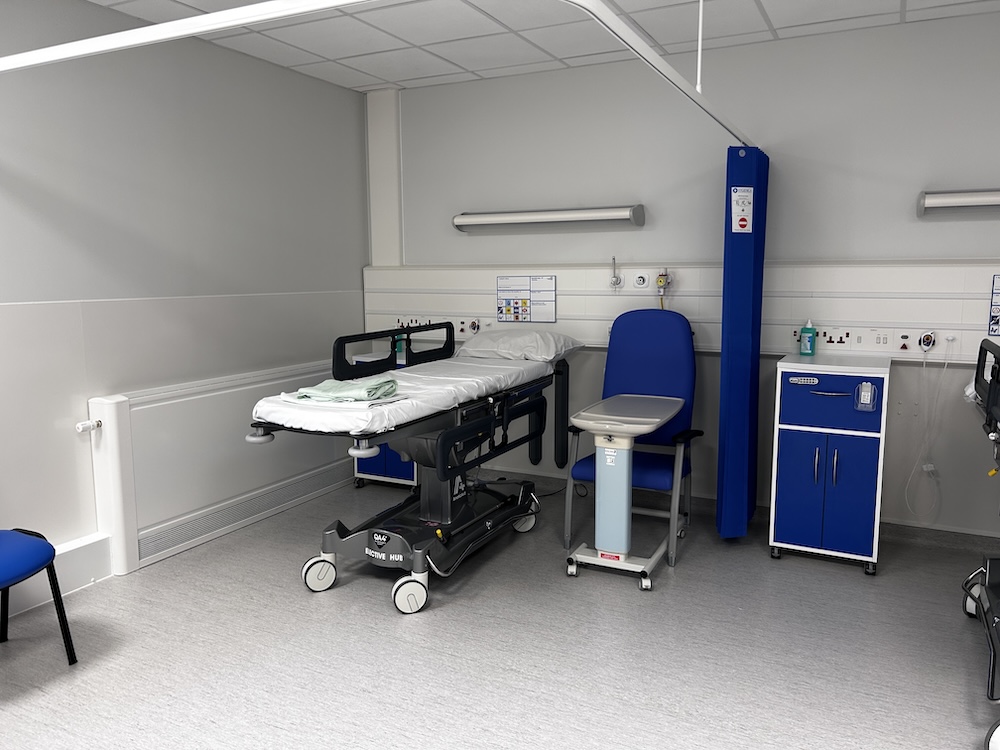
Construction work is well underway at Royal Shrewsbury Hospital to build a new four-storey building which will provide the space we need to start our new ways of working. We’re also investing in services at Princess Royal Hospital in Telford to provide a more positive experience for patients in calm, dedicated planned care facilities.
How will this improve care for our patients
What is changing at our hospitals?
Princess Royal Hospital in Telford will become the site specialising in planned care. Patients will have a more positive experience in improved, dedicated planned care facilities.
Royal Shrewsbury Hospital will become the site specialising in emergency care. All the right doctors and nurses who support our emergency care teams will be on the same site as the remodelled Emergency Department. This means they can make quicker decisions about your care.
Most patients will continue to use their local hospital, including for outpatient appointments and urgent care services. Most people that currently use our Emergency Department (A&E) will use the Urgent Treatment Centre at their local hospital.